The Medical Management Platform for Modern Payers
Unify prior authorization, care management, and member engagement in one platform built for payers under pressure.
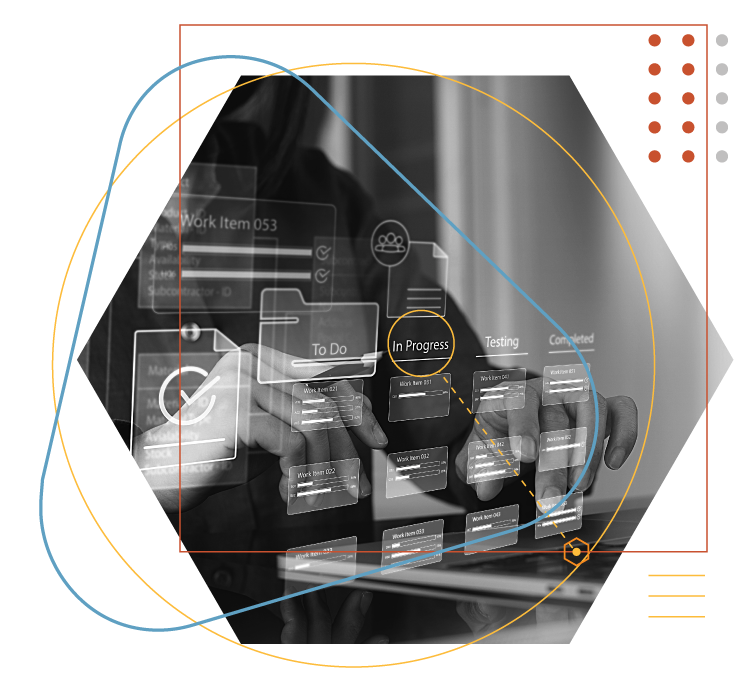
From CMS-0057-F and Star Ratings to redeterminations and risk adjustment, Helios® by Elligint Health helps Medicare Advantage, Medicaid Managed Care, and commercial health plans streamline operations, act earlier on risk, and coordinate care more efficiently as networks, models, and mandates evolve.
Elligint Health delivers a purpose-built ecosystem designed to help health plans perform with confidence across every contract and population. At the center of that ecosystem are three key capabilities:
Advanced Analytics by Elligint Health
Delivering predictive insights and performance intelligence across clinical, operational, and financial data.
Helios Partner Ecosystem by Elligint Health
Expanding platform capabilities through seamless integrations with specialized partner technologies — without adding complexity.
Built for Performance
Payers today face relentless pressure — regulatory mandates, medical cost containment, member experience expectations, and legacy technology that can’t keep up. Performance isn’t about doing more work — it’s about removing the friction that slows decisions, delays care, and inflates administrative costs. Helios helps you:
- Speed Care Management interventions using smart workflows
- Reduce manual interventions with automated workflows leveraging AI
- Accelerate turnaround times for prior authorizations, grievances, and appeals
- Improve care team productivity without adding staff
- Lower administrative spend tied to redundant systems
- Align with CMS-0057-F using audit-ready workflows and regulatory compliance tracking
With Helios, You Can:
- Unify information systems across healthcare continuum using FHIR-native data exchange
- Automate CM and UM workflows for faster turnaround times — no more manual workarounds
- Identify rising-risk and rising-cost members early using AI with predictive analytics
- Use built-in assessments to gather patient data or build your own using our Assessment Tool Builder featuring branching, mapping, and auto-population logic
- Engage members and coordinate whole-person care across clinical and social needs
Recognized. Proven. Preferred.
Elligint Health isn’t just a vendor—we’re a partner in performance.
- Proven support for whole-person care planning and risk-based coordination
- Automation across prior authorizations, grievances, and appeals workflows
- Configurable workflows designed to reduce administrative burden
- FHIR-native interoperability across your technology ecosystem
- Integrated telehealth and member outreach tools


One Platform. Endless Impact.
- Recognized as a top performer by KLAS Research
- One system for care and utilization management
- 90% configurable to align with your contracts and processes
- Real-time operational insights that prioritize and drive action
- Increased productivity & reduced administrative burden
- Over 13M lives managed and industry-leading retention
Ready to Perform Under Pressure?
Whether you’re managing Medicaid redeterminations, scaling Medicare Advantage, or expanding commercial VBC contracts—Elligint Health helps you do it with clarity, speed, and measurable impact.

